Post-Surgical Pain After Tubal Ligation or Reversal
Tubal ligation is often considered a minor procedure, and for most women, recovery is straightforward. But for some, persistent pelvic or abdominal pain develops afterward and is frequently dismissed as unrelated to the surgery. It often isn’t.
Dr. Richard Nahas helps patients in New York City uncover the nerve and fascial changes that can drive ongoing pain after tubal ligation or reversal.
What you might be feeling
- Pelvic or lower abdominal pain
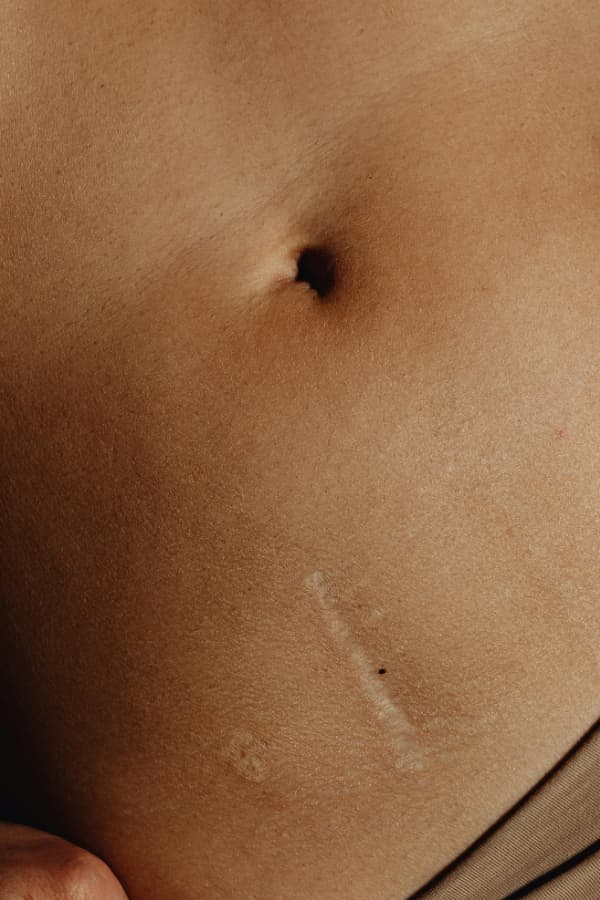
- Trocar site tenderness or sensitivity
- Unexplained groin discomfort
- Burning or sharp sensations near incisions
- Pain that developed shortly after surgery
- Lower back aching
- Discomfort with activity or prolonged standing
Why the pain persists
Because tubal ligation is laparoscopic and considered low-risk, ongoing pain is often attributed to other causes or dismissed entirely. But even small incisions and subtle tissue manipulation in the pelvis can create meaningful nerve and fascial changes that generate chronic symptoms.
Trocar site nerve irritation
Small sensory nerves in the abdominal wall pass directly through the trocar sites. Compression, stretching, or entrapment during healing can leave these nerves persistently sensitized, producing sharp or burning pain at the port sites.
Fascial restriction near the tubes
Manipulation and cauterization of the fallopian tubes create local tissue changes that extend into the surrounding fascia. These restrictions can alter pelvic mechanics and generate discomfort that radiates into the groin or lower abdomen.
Scar tissue at surgical sites
Even minor laparoscopic procedures can produce scar tissue that becomes an interference field, maintaining abnormal nerve signaling long after the visible incision has healed.
Post-reversal tissue complexity
Tubal reversal involves more extensive repair and carries a higher likelihood of adhesion formation and nerve disruption. Pain after reversal may reflect both the original ligation site and new tissue changes from the reconstruction.
How Dr. Nahas approaches it
Dr. Nahas takes post-tubal pain seriously, even when others don’t. Using his Blockage-Based Care framework, he performs a detailed assessment to identify the specific tissue and nerve contributors and builds a treatment plan around those findings rather than a general pain management approach.
- Scar & fascial assessment — Hands-on examination to identify trocar site sensitization, fascial restrictions, and interference fields in the lower abdomen and pelvis.
- Neural therapy — Targeted injections at scar-related interference fields to normalize abnormal nerve signaling at and around the surgical sites.
- Peripheral nerve blocks — To identify and treat sensitized nerves contributing to pelvic, groin, or abdominal wall symptoms.
- Trigger point & regenerative tools — Restoring tissue balance and addressing any compensatory strain patterns in the surrounding pelvic structures.
Still in pain after tubal ligation or reversal?
Book Your Virtual or In Person Consultation
If you’ve been told your pain isn’t related to your procedure, it may be time for a second opinion. Dr. Nahas offers comprehensive evaluations for women experiencing persistent symptoms after tubal surgery — at his Manhattan office, with no referral required.